You are here
- Home >
- Departments & Centers >
- Pulmonary, Allergy, and Critical Care >
- About Us >
- Our History
Our History
Until 1968, most patient care and research in pulmonary medicine were carried out by the Chest Service of the Columbia University Division at Bellevue Hospital. After 1968, the Columbia pulmonary faculty moved to Washington Heights and Columbia-Presbyterian Medical Center.
-
1932
Dickinson Richards Established a Cardiopulmonary Laboratory With André Cournand

In 1932, Dickinson Richards established a cardiopulmonary laboratory with André Cournand, with whom he collaborated for 40 years. Together, they advanced the concept of the heart and lungs as a single integrated physiological system. Their work on cardiac catheterization revolutionized medicine and helped pave the way for cardiac bypass surgery. In 1956, Drs. Richards and Cournand, together with Werner Forssmann, received the Nobel Prize in Physiology or Medicine.
-
1962
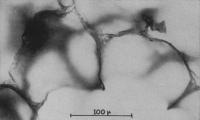
Drs. Ewald Weibel and Domingo Gomez Conducted Landmark Studies on Lung Morphology and Morphometry

In 1962, Drs. Ewald Weibel and Domingo Gomez conducted landmark studies on lung morphology and morphometry. Their work applied quantitative methods to the study of lung structure, providing a systematic framework for measuring the architecture of the lung. These studies helped establish modern approaches to understanding the relationship between lung structure and respiratory function.
-
1970
Dr. Yale Enson Conducted Important Studies Describing the Physiological Mechanisms Underlying Pulmonary Hypertension
In the 1970s, Dr. Yale Enson, who trained in André Cournand’s laboratory, conducted important studies describing the physiological mechanisms underlying pulmonary hypertension. Over a distinguished career, he made significant contributions to the understanding of pulmonary vascular disease. Dr. Enson retired in 1999 after 38 years of service (1961–1999) to the Division.
-
1973
Dr. Réjane M. Harvey Appointed Director of the Pulmonary Division at Presbyterian Hospital

In 1973, Dr. Réjane M. Harvey served as Director of the Pulmonary Division at Presbyterian Hospital. A cardiopulmonary physiologist, she was a member of the Columbia University faculty for 37 years (1946–1983) and also served as Chief of the Division of Cardiology at Harlem Hospital (1968–1983). In 2002, she received the Distinguished Service Award, the highest honor awarded by the College of Physicians and Surgeons.
-
1983
Dr. P. R. B. Caldwell Appointed Chief of the Pulmonary Division
In 1983, Dr. P. R. B. Caldwell became Chief of the Pulmonary Division. He and his colleagues purified angiotensin-converting enzyme (ACE) from rabbit lungs and demonstrated its localization in the vascular endothelium, advancing the understanding of the pulmonary circulation and the biological role of ACE.
-
1997
Dr. Paul Rothman Appointed Chief of the Pulmonary Division

In 1997, Dr. Paul Rothman became Chief of the Pulmonary Division. A molecular immunologist, his research focused on cytokine signaling and immune system responses related to allergy, asthma, and inflammatory lung disease. During his tenure, the Division added Allergy as a subspecialty and expanded its leadership in Critical Care Medicine.
-
2005
Dr. Neil Schluger Appointed Chief of the Division

Neil Schluger, MD
In 2005, Dr. Neil Schluger (include picture) was appointed Chief of the Division. His research focused on the epidemiology, diagnosis, and treatment of tuberculosis. During his tenure, the MICU program and several outpatient programs expanded, and the Jo-Ann LeBuhn Center for Chest Disease and Respiratory Failure and the Price Family Comprehensive Center for Chest Disease were established in collaboration with the Division of Thoracic Surgery.
-
2020
Dr. Christine Kim Garcia Appointed Chief of the Division

Christine Kim Garcia, MD, PhD
In 2020, Dr. Christine Kim Garcia was appointed Chief of the Division. Her laboratory’s research has focused on identifying genetic contributors to pulmonary fibrosis, including telomere shortening and surfactant dysfunction. Under her leadership, the Division expanded to include an Interventional Pulmonary Program and the Claire Tow Home Assisted Ventilation Program.